Patient Information
Procedures
- Colonoscopy
- What is a colonoscopy? A colonoscopy is a camera test – using a flexible tube with a light and lens on the end, it is inserted into the rectum and advanced through the colon to the small bowel. We use this test for diagnostic purposes – to find polyps, abnormalities, etc.
- Why should I get one?
- If you have a family history of colon cancer or colon polyps, or if you are experiencing symptoms of concern such as changes in your bowel habits, pain, or rectal bleeding, you should speak with your doctor about scheduling a colonoscopy. In order to do this test, you must complete a bowel preparation that will clean out your colon. Please see the patient preparation page for more information. Are there any risks to this procedure? With any procedure, there are risks of complication, but they are rare.
- Minor risks: Bloating, abdominal discomfort, medication reactions or temporary minimal bleeding.
- Major risks: perforation or hole in the colon which would require a surgical repair or heavy bleeding requiring intervention.
- Gastroscopy
- What is a Gastroscopy? A Gastroscopy is a camera test- using a flexible tube with a light and lens on the end, it is inserted into the mouth, down the esophagus into the stomach and beginning of the small bowel. We use this test for diagnostic purposes – to find abnormalities and sample tissues.
- Why should I get one? If you are experiencing indigestion, nausea, or difficulty swallowing, you should speak with your doctor about scheduling a gastroscopy. Preparation instructions for this test include fasting (instructions provided to patients) Are there any risks to this procedure? With any procedure, there are risks of complication, but they are rare.
- Minor Risks: Discomfort, pain in the upper GI tract, medication reactions, or temporary minimal bleeding
- Major Risks: Perforation or hole in the digestive tract which would require a surgical repair or heaving bleeding requiring intervention.
- Flexible Sigmoidoscopy
- What is a flexible sigmoidoscopy? A flexible sigmoidoscopy is a camera test- using a flexible tube with a light and lens at the end, it is inserted into the rectum and up to the sigmoid colon. We use this test to look at a very small section of the colon. These tests are only done in special circumstances where a complete colonoscopy is not necessary. In order to do this test, you must complete a bowel preparation that will clean out the end of your colon. Please see the patient preparation page for more information.
Preparation Instructions
If you are scheduled for a colonoscopy, you will be required to complete a bowel cleanse. A bowel cleanse is a solution used to empty your colon. There are different types of cleanses available at the pharmacy. Our team will provide you with the preparation instructions including which preparation your doctor would like you to use.
**Please do not use these bowel cleansers unless you are booked for a procedure**
How do I know I’m prepared or cleaned out enough?
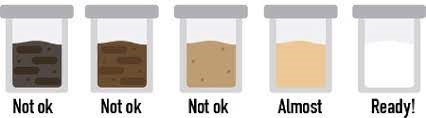
You are prepared when your bowel movements are clear in color and the consistency of urine. If your bowel movements are still murky after completing the preparation, please call the office.
What to Expect
Your doctor or nurse practitioner will send a referral to our clinic. This referral gets triaged by our team. If your referral has been cleared, we will then call or email to book you in for your appointment. If you have a number of medical conditions & medications, you will be required to complete a consultation with our Internal Medicine physician’s prior to booking in for a procedure. Our internal medicine physicians complete a physical assessment & provide instructions for managing medications prior to undergoing a procedure.
Please bring with you a valid health card, a list of your current medications, a completed patient questionnaire & the name and phone number of the responsible adult who will either be picking you up or accompanying you home from your procedure.
All procedure patients will have an intravenous access (IV) prior to procedure, regardless if they choose to forego sedation. An IV access allows our team to intervene quickly should there be an emergency.
Why do I need a responsible adult to drive me home or accompany me home?
- You will be offered IV sedation to keep you comfortable during your procedure. If you choose to use the sedation you will be considered legally impaired. You will not be able to drive, drink alcohol, or sign any legal documents for up to 24 hours.
- If you choose to take a taxi, Uber, bus or ParaTranspo, you must have a responsible adult accompany you because the drivers alone are not responsible for your wellbeing.
- If you choose not to have sedation, you must come prepared with your emergency name & contact number.
You can expect to be at the facility from 1 hour up to 3 hours. Unfortunately, we cannot predict when there may be delays, but we treat every patient with the care and attention they deserve. We appreciate your patience while you wait.
Once you are admitted into a bed, your team will set you all up & once the physician is ready, your team will escort you to the procedure room where you’ll meet your endoscopist & get a chance to discuss the procedure.
Your results will be given to you immediately following your procedure. Our recovery room team will review your discharge instructions & results. Since the side effects of the medication you received may cause you to forget, you will also receive a written report for your own records. Any samples removed will be sent out to the lab for analysis & your family doctor will receive those results in 4 weeks.
Clinic Policies
- Cancellation Policy:
- Our office requires a minimum of 7 business days’ notice to cancel or reschedule an appointment. If sufficient notice is not provided, a $250+tax fee may apply (at the discretion of the physician).
- Covid Policy (if applicable)
- Zero Tolerance Policy:
- We will not tolerate any inappropriate behavior towards any member of staff or patients alike. This includes but is not limited to verbal abuse, aggression, physical abuse, or disruptive behavior. Anyone found in violation of such will be asked to leave immediately & will no longer be welcome as a patient of OGI. Thank you for being so cooperative in keeping our environment safe.

- NPO Policy:
- All patients arriving for a procedure must refrain from drinking for 4 hours before their test. See FAQ
- IV Access:
- All patients arriving for a procedure will have intravenous access, even if they do not wish to have sedation. This is a safety concern & allows our team to intervene quickly should an emergency arise.
- Ride Policy:
- Our patients are required to have a responsible adult drive them or accompany them home. For patients booked at the end of the day, rides should be waiting in the waiting room by no later than 4pm.
Frequently Asked Questions
We ask that you temporarily alter your diet 5 days before to avoid nuts and seeds as these food items stick to the walls of your colon and are difficult to flush out with the bowel preparation. They may prevent your doctor from getting a proper visualization of your tissues & they can also damage the equipment. Please avoid fruits & vegetables with seeds, whole grains, oatmeal, flax seed, & crunchy peanut butter in the 5 days leading up to your colonoscopy.
We ask that you do not eat any solid foods the day before your test and the day of your procedure until your scope is completed because food creates solid stool. You are on a clear fluid diet only beginning the day before your procedure so that the bowel cleanse can properly clear out your colon, allowing the doctor to be able to properly assess your colon.
A clear fluid is any type of fluid that you can see through such as water, apple juice or Jell-O. Please do not drink dairy products or drinks that you cannot clearly see through.
Please do not consume coffee, coconut water, broth or tea while completing your cleanse.
Yes. Regardless if you experience diarrhea frequently or are petite, the bowel cleanse must be completed in full.
We ask that you do not consume anything by mouth 4 hours before your test to ensure that your stomach is empty. While under sedation, stomach contents are at risk of coming up into your lungs. This is considered a medical emergency. Fasting is for your own safety. If you do not fast, you risk your appointment being delayed and/or cancelled by our anesthesia team.
We ask that you avoid travelling out of the country or by airplane for at least 7 days after your procedure in case you experience a complication. Complications can arise, post procedure anywhere from up to 7 days after the procedure.
A FIT test detects blood in your stool. If you have a personal history of Crohn’s Disease, Ulcerative Colitis or colon polyps, and/or a family history of colon cancer, or symptoms such as bleeding or changes in your bowel habits, then a FIT test is not appropriate for you.
Patients deemed average risk above age of 50 without any symptoms of concern are suitable for a FIT test or a colonoscopy. It is up to you, as the patient to discuss with your family doctor which test is suitable for you.
When in doubt, a colonoscopy is the best line of defense in preventing colon cancer. It allows a good visual of the tissues and the ability to remove small polyps before they develop into cancer, which would not be identified on a FIT test.
If a FIT test result comes back positive, that means there is blood present in your stool. A colonoscopy must be performed urgently to determine where the blood is coming from. This is no necessarily indicative of cancer, or may indicate hemorrhoids, inflammatory bowel disease, diverticulosis or large polyps. Your family physician can refer to OGI’s RAS (Rapid Access Service) to ensure your colonoscopy will be prioritized and completed within weeks.
Polyps are growths that can form in the colon. There are several different types and sizes of polyps. Some are harmless and some have the potential to turn into cancer. During a colonoscopy, your doctor will remove the polyps they find & send them to the laboratory for analysis. Removing them in the smaller stages prevents them from growing & potentially forming into cancer.
Visual Aid
Once you’ve had polyps, you will be scheduled for colonoscopies at regular intervals to prevent the development of cancer.
Inflammatory bowel disease is an umbrella term used to describe two different disorders that affect the GI tract. Crohn’s Disease and Ulcerative Colitis are disorders that involve chronic inflammation in the GI tract. Prolonged untreated inflammation can lead to damage of the GI tract. Symptoms include abdominal pain, diarrhea and bloody stool.
Crohn’s Disease is a chronic inflammatory disorder than can affect any part of the GI tract from the mouth to the rectum, but it most commonly affects the small bowel & beginning of the large intestine.
Crohn’s Disease tends to have relapsing and remitting flare-ups and require on-going follow up by a gastroenterologist.
Ulcerative Colitis is a chronic inflammatory disorder that only affects the large intestine and rectum. It is characterized by inflammation and ulcers that line the intestine.
Ulcerative Colitis tends to have relapsing and remitting flare-ups and require on-going follow up by a gastroenterologist.
Hemorrhoids are swollen blood vessels in the rectum. Occasionally, hemorrhoids can bleed, especially after frequent or large bowel movements. There are treatments available to manage symptoms from hemorrhoids.
As we age, the walls of our colon weaken, forming pouches known as “diverticuli”. These pouches or diverticuli can fill with stool & cause pain. It is a common condition; approximately 50% of the population has diverticulosis after the age of 60.
Occasionally, these pouches become infected (known as diverticulitis) and will require antibiotic treatment. If you’ve had a recent flare up of diverticulitis, your colonoscopy should be delayed until you’ve recovered.
